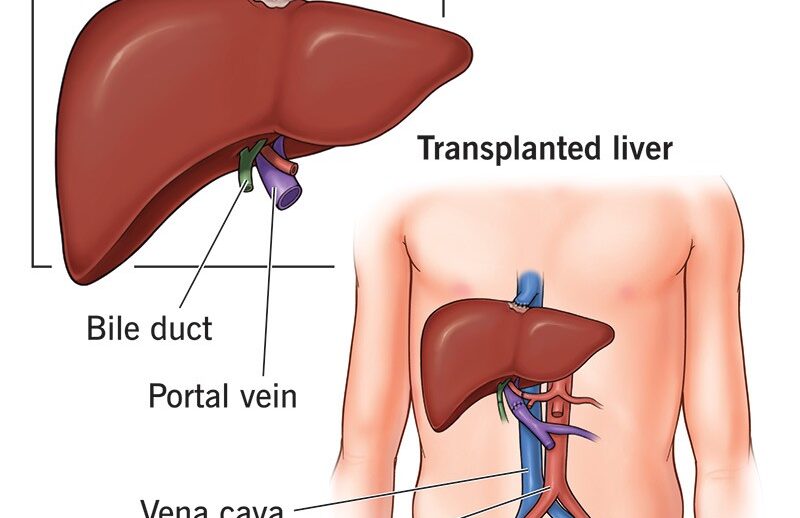
A liver transplant is a major surgical procedure that replaces a diseased, failing liver with a healthy one from a deceased or living donor. It is primarily used to treat acute liver failure or end-stage chronic liver disease (cirrhosis). The surgery involves removing the diseased liver, typically lasting 5-8 hours, and offers high survival rates.
Key Aspects of Liver Transplant:
- When It’s Needed: It is required for irreversible end-stage liver disease or acute liver failure. Common causes include chronic hepatitis, alcoholic liver disease, fatty liver disease, and liver cancer.
- Types of Transplant:
- Deceased Donor Transplant (DDLT): The most common type, where a whole liver is obtained from a deceased donor.
- Living Donor Transplant (LDLT): A portion of a healthy person’s liver is removed and transplanted into a recipient. Because the liver can regenerate, both the donor’s and recipient’s livers will grow back to normal size.
- The Procedure: Surgeons perform a large, T-shaped or rooftop incision to remove the old liver and connect the new liver to the patient’s blood vessels and bile ducts.
- Post-Operative Care: Patients are transferred to the ICU for monitoring to prevent organ rejection. Lifelong immunosuppressant medications are necessary to prevent the body from attacking the new liver.
- Success Rates & Recovery: For deceased donor transplants, survival rates are approximately 86% at 1 year and 78% at 3 years. Most patients return to a normal, active life within one year.
- Waiting List: Candidates are evaluated and placed on a waiting list managed by organizations like UNOS, where priority is determined by the MELD score (Model for End-Stage Liver Disease), which measures the severity of the illness.