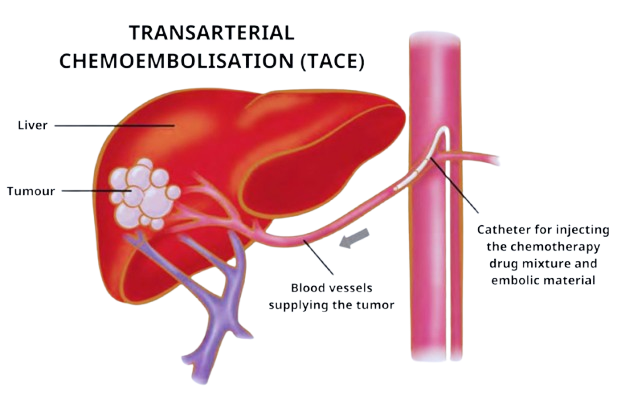
Transarterial Chemoembolization (TACE) is a minimally invasive, targeted treatment for liver cancer (especially Hepatocellular Carcinoma) that combines chemotherapy with vessel blockage. By injecting chemo drugs directly into the liver tumor’s artery, it kills tumor cells while starving them of oxygen, minimizing systemic side effects compared to traditional chemotherapy.
Key Details About TACE
- How it Works: A catheter is inserted through the groin and guided by X-ray to the liver artery. Doctors inject chemotherapy agents (often mixed with oily contrast) followed by embolizing particles (e.g., gelatin sponge, drug-eluting beads) to cut off the tumor’s blood supply.
- Target Population: Primarily for patients with large or multiple, unresectable hepatocellular carcinoma (HCC) without vascular invasion or spread outside the liver. It is also used to “bridge” or “downstage” patients waiting for a liver transplant.
- Types: Conventional TACE (cTACE) uses oil-based chemotherapy, while Drug-Eluting Bead TACE (DEB-TACE) uses beads that slowly release chemotherapy for potentially fewer side effects.
- Procedure & Recovery: Usually an outpatient or short-stay (1-2 days) procedure.
- Side Effects: Common side effects include pain, nausea, vomiting, low-grade fever (post-embolization syndrome), fatigue, and loss of appetite.
- Effectiveness: It is highly effective for reducing tumor size and improving survival in intermediate-stage, non-surgical candidates.